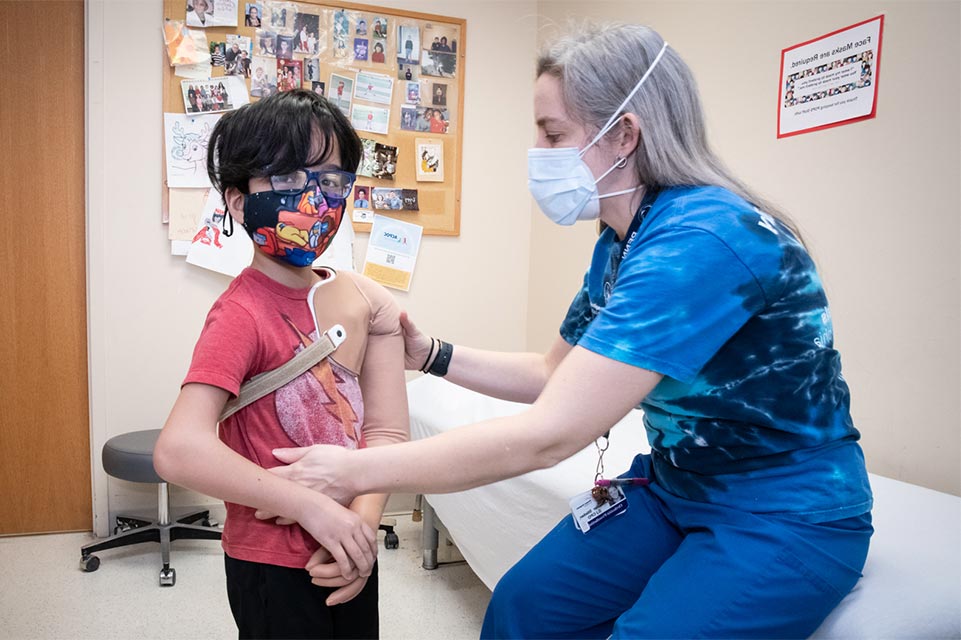
Orthopedics
Families seeking specialty orthopedic care for children come to Shriners Children’s.
Across our healthcare system, we offer the full spectrum of orthopedic treatments and services – from fracture care and casting for broken bones, to surgery and rehabilitation. We also provide low-dose radiology, motion analysis, bracing, casting, and orthotic and prosthetic services. All of these are complemented by our physical, occupational and recreational therapy programs. Families appreciate the convenience of a single source for treatment, and children benefit from the continuity of care and collaboration. With this collaborative approach, parents, patients and providers can all support the total care plan.
We’re proud that U.S. News & World Report ranked six of our locations among the "best children’s hospitals for orthopedics" in the United States in 2020. We celebrate the recognition of our individual physicians and researchers, as well. The American Academy of Orthopaedic Surgeons, the American Academy for Cerebral Palsy and Developmental Medicine, the Pediatric Orthopedic Society of North America, and the American Academy of Pediatrics are just a few of the organizations that have honored our staff.
Our pediatric orthopedic specialists gain much of their expertise through hands-on experience, individualized education and concentrated research with organizations including universities and companies in the private sector. As a result of this self-directed training, they’ve developed the elite skills to treat more than 100 orthopedic conditions.
Because Shriners Children’s provides all care and services regardless of a family’s ability to pay or insurance status, physicians and families are able to consider every appropriate treatment option available. Learn more below about the pediatric orthopedic conditions we treat and our commitment to the overall well-being of your child.
Specific treatments and services may vary by location. Please contact a specific location for more information.
Orthopedic Conditions Treated at Shriners Children’s
Our pediatric orthopedic physicians are among the most highly skilled and specialized in North America. The types of conditions we treat vary by location, and the following is not a complete list.
If you do not see your child’s condition, please search all orthopedic conditions or contact the Shriners Children's location nearest you.
Amputation
Bone Defects/Disease
- Congenital pseudoarthrosis
- Osteochondritis dissecans (OCD lesions)
- Osteogenesis imperfecta (OI)
Bowed Legs
- Blount’s disease
- Physiologic
- Rickets
Dwarfism
Finger Conditions
- Absent digits
- Macrodactyly
- Polydactyly (extra fingers or toes)
- Syndactyly (webbed fingers or toes)
Foot Conditions
- Bunions (halux valgus)
- Cavovarus
- Clubfoot
- Foot pain
- Skew foot (metatarsus adductus)
- Pes cavus (high arch)
- Pes planus (flat feet)
- Tarsal coalition
- Toe-walking
Fractures
- General fractures
- Complications after fractures
- Non-emergent follow-up
Hand Conditions
- Congenital hand anomalies
- Radial anomalies (club hand, hypoplasia)
- T.A.R. syndrome (thrombocytopenia absent radius)
Hip Deformities
- Hip dysplasia (hip dislocation)
- Femoroacetabular impingement (FAI)
- Legg-Calve Perthes disease
- Slipped capital femoral epiphysis (SCFE)
Knee Conditions
- Anterior cruciate ligament injury (ACL)
- Genu valgum (knock knees)
- Meniscus injury
- Osgood-Schlatter disease
Leg-length Discrepancies
Miscellaneous Orthopedic Conditions
- Abnormal gait (walk)
- Amniotic band syndrome
- Arthrogryposis
- Benign tumors/cysts of the bone
- Solitary and multiple hereditary exostosis (osteochondromatosis)
Neck Conditions
- Klippel-Feil syndrome
- Torticollis
Shoulder Conditions
- Erb’s palsy (brachial plexus palsy)
- Sprengel’s deformity
Spine Conditions
Toe Conditions
- Macrodactyly
- Polydactyly (extra toes or fingers)
- Syndactyly (webbed toes or fingers)
How We Support Your Child’s Total Health and Well-Being
Families and patients say that Shriners Children’s feels like home to them, and it's no wonder to us. We know that a child's needs go beyond the physical. Our care teams support their social, emotional and developmental health with patient programs and activities.
A few examples include:
- Child life enrichment
- Creative arts
- Live entertainment
- Music therapy
- On-site public schooling
- Pet therapy
- School and community re-entry program
- Specialty camps
- Therapeutic recreation
Not all programs are available at every location. Contact your child’s care manager or any member of your child’s care team to learn more.

The hospital feels like home to me. I love being around other kids who are overcoming obstacles in life like me.

More than Measurements and Mechanics
Innovative Treatments
View All Related Treatments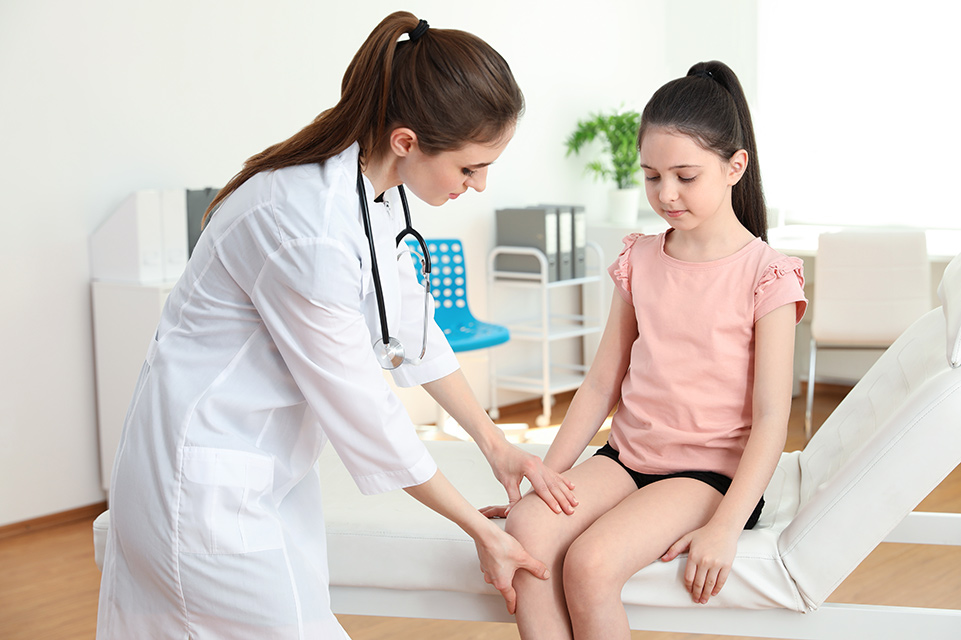
Bracing

Casting
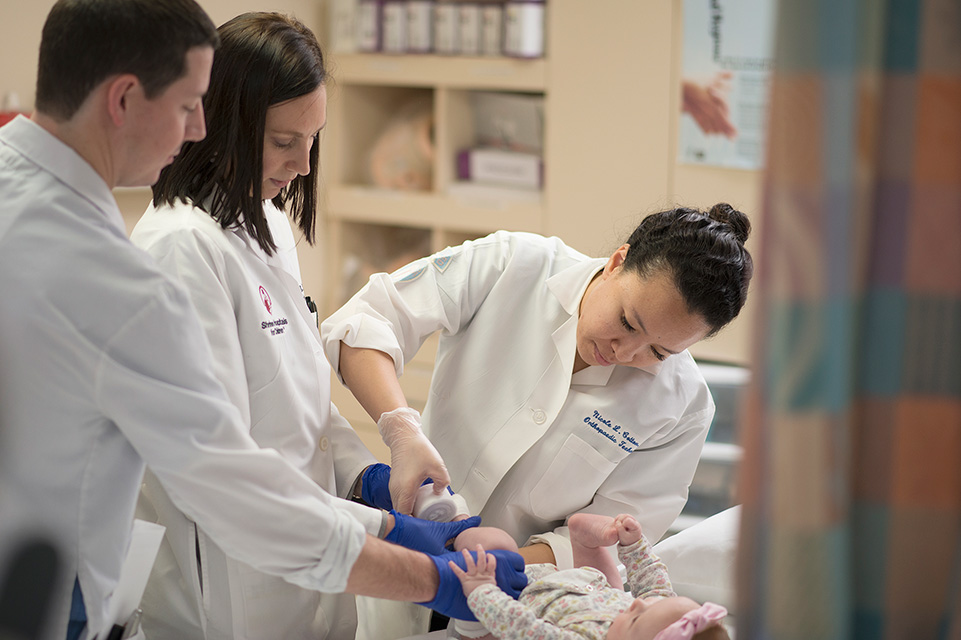
Growing Rods
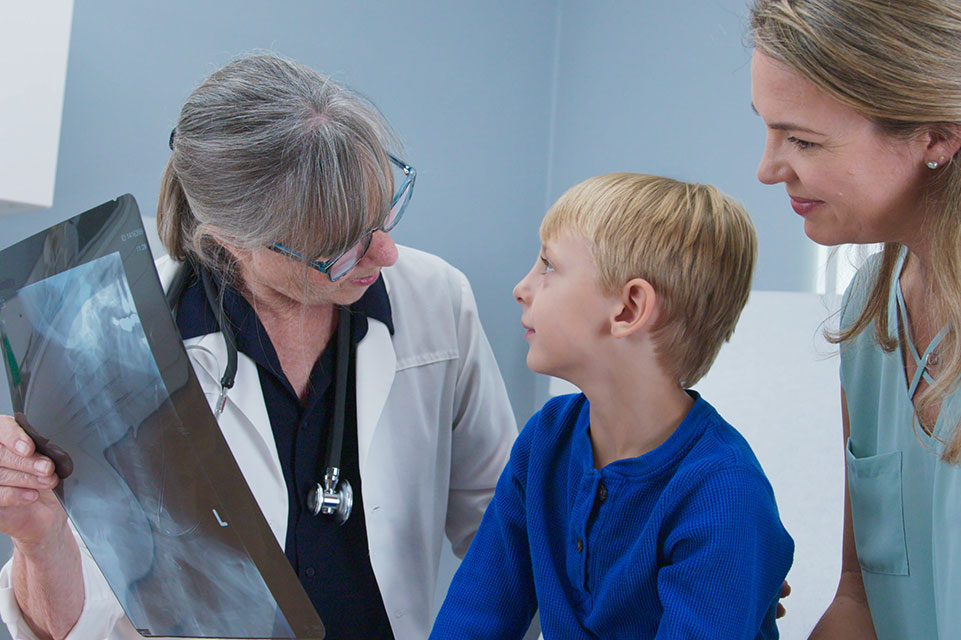
Laser Surgery

Limb Lengthening

Physical Therapy
Reconstructive Surgery