Craniofacial Care
At Shriners Children’s, families find internationally recognized craniofacial care, hope and compassion.
Sometimes a new baby or adopted child has a difference in their smile or the shape of their face, nose or chin, known as a craniofacial (head and face) difference. Conditions can range from mild to severe.
Shriners Children’s specialists can help with the physical, social, emotional and developmental challenges that occur when a child has a congenital (present at birth) or acquired (develops later) condition. We provide a team approach at child-friendly facilities, where multiple specialists see the child all in one day. It is our goal to make medical care convenient and friendly for the child and parent.
Shriners Children’s locations offer advanced treatments and services such as craniofacial surgery, 3D printing for jaw surgeries, facial and dental imaging, psychology, speech therapy, audiology, ear, nose and throat surgeons, dental and orthodontic related services, and care management. Our family-centered approach celebrates the journey of each patient, inviting the parent to collaborate with specialists to create the best treatment plan for their child.
We are proud that multiple Shriners Children’s locations are American Cleft Palate Craniofacial Association approved teams. Our plastic surgeons have undergone additional training to evaluate and treat craniofacial conditions in children.
Because Shriners Children’s provides all care and services regardless of a family’s ability to pay or insurance status, physicians and families are able to consider every appropriate treatment option available. Learn more below about the pediatric craniofacial conditions we treat and our commitment to the overall well-being of your child.
Specific treatments and services may vary by location. Please contact a specific location for more information.
Specialized Care as Your Child Grows
Care for your child may begin and end in infancy, or continue until they are fully grown. Our doctors and specialists are even available to consult with parents who are adopting, or expecting a baby who has been diagnosed in utero, with a craniofacial difference; for example: cleft lip/cleft palate.
Many craniofacial differences will require multiple surgeries to improve the way a child’s face and head looks and functions. Our surgical techniques minimize visible scars and help patients enjoy a normal full life.

The staff was so friendly and helpful. The Cleft/Craniofacial team provided all the information, support and level of specialized care that we were seeking.
Craniofacial Conditions We Treat
Shriners Children’s provides care for hundreds of craniofacial conditions and syndromes. The types of conditions we treat vary by location. These are conditions we commonly see in children:
- Cleft Lip
- Cleft Palate
- Craniofacial Microsomia
- Goldenhar Syndrome/Hemifacial microsomia
- Differences in babies’ ears, head shape and face shape
- Craniofacial anomalies associated with congenital syndromes such as 22q11.2 deletion, Crouzon, Apert, Pfieffer or Treacher-Collins.
- Chronic wounds (wounds that won't heal), such as pressure wounds
- Dog Bites
Our plastic surgery team can also provide care for other conditions such as jaw deformities, vascular malformation /nevi, and hemangioma.
Plan Your Visit
Families are amazed that at Shriners Children's they see so many specialists in one place, all focused on their child. The craniofacial team meets together several days per week to coordinate treatment planning across the specialties, to help kids live their absolute best lives, no matter where they are in the course of treatment. Your child will likely see the entire team of specialists once or twice per year.
After checking in, you will be escorted to your exam room. All the specialists your child needs to see that day will come to you. This may include plastic surgeons, oral maxillofacial surgeons, ear, nose and throat doctors, psychologists, orthodontists and dentists, speech pathologists, pediatric nurses/nurse practitioners and clinical dietitians. Care managers (RNs and social workers) are available to help patients and families find resources they need during the child’s various stages of care.
Families should be prepared to spend several hours for full-team appointments. After each team appointment, you will receive a multidisciplinary team report to take to your child's doctors at home.
In some cases, telehealth appointments may be available to bring our specialty care to where you are.

Giving Children Comfort and Coping Skills
Services We Provide
View All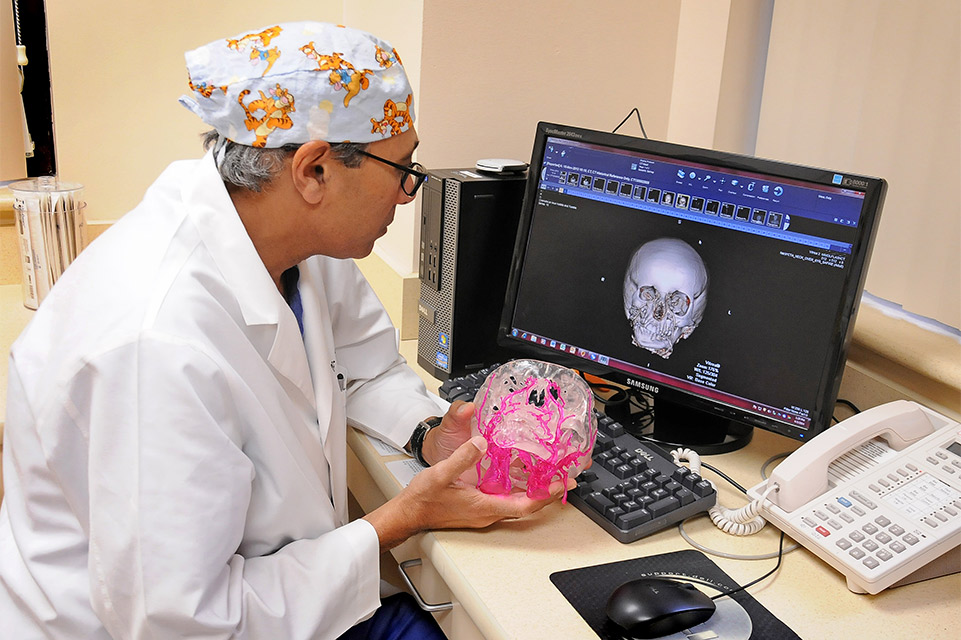
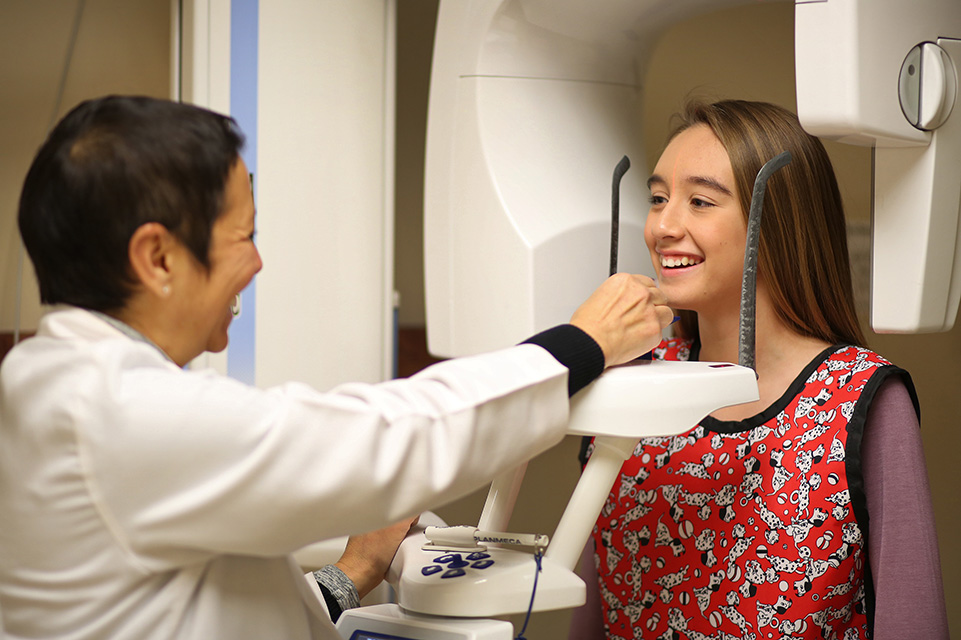
Facial and Dental Imaging
Dentistry

Ear, Nose, Throat Services

Speech Therapy
Care Management

Psychiatry & Psychological Services

School and Community Re-entry Program

Related Treatments
- Craniofacial Surgery
- Helmet Therapy
- Physical Therapy
- Newborn Ear Molding
- Plastic Surgery
- Prosthetics and Orthotics
- Reconstructive Surgery
- View All Craniofacial Treatments
Related Conditions
- Atypical Head Shape
- Cleft Lip
- Cleft Palate
- Craniofacial Microsomia
- Dentofacial Skeletal Deformity
- Jaw Deformities
- Microtia
- View All Craniofacial Conditions